New survey finds that talking therapies have the greatest positive impact on mental health
What impact has COVID-19 had on mental health? And have people been able to receive effective mental health support?
To answer these questions, we worked in partnership with YouGov to poll a representative sample of 2,000 UK adults. It is important to us that UKCP’s work is informed by people’s real-world experience and we were hoping to demonstrate the positive impact of psychotherapy and counselling on mental health.
Key Findings
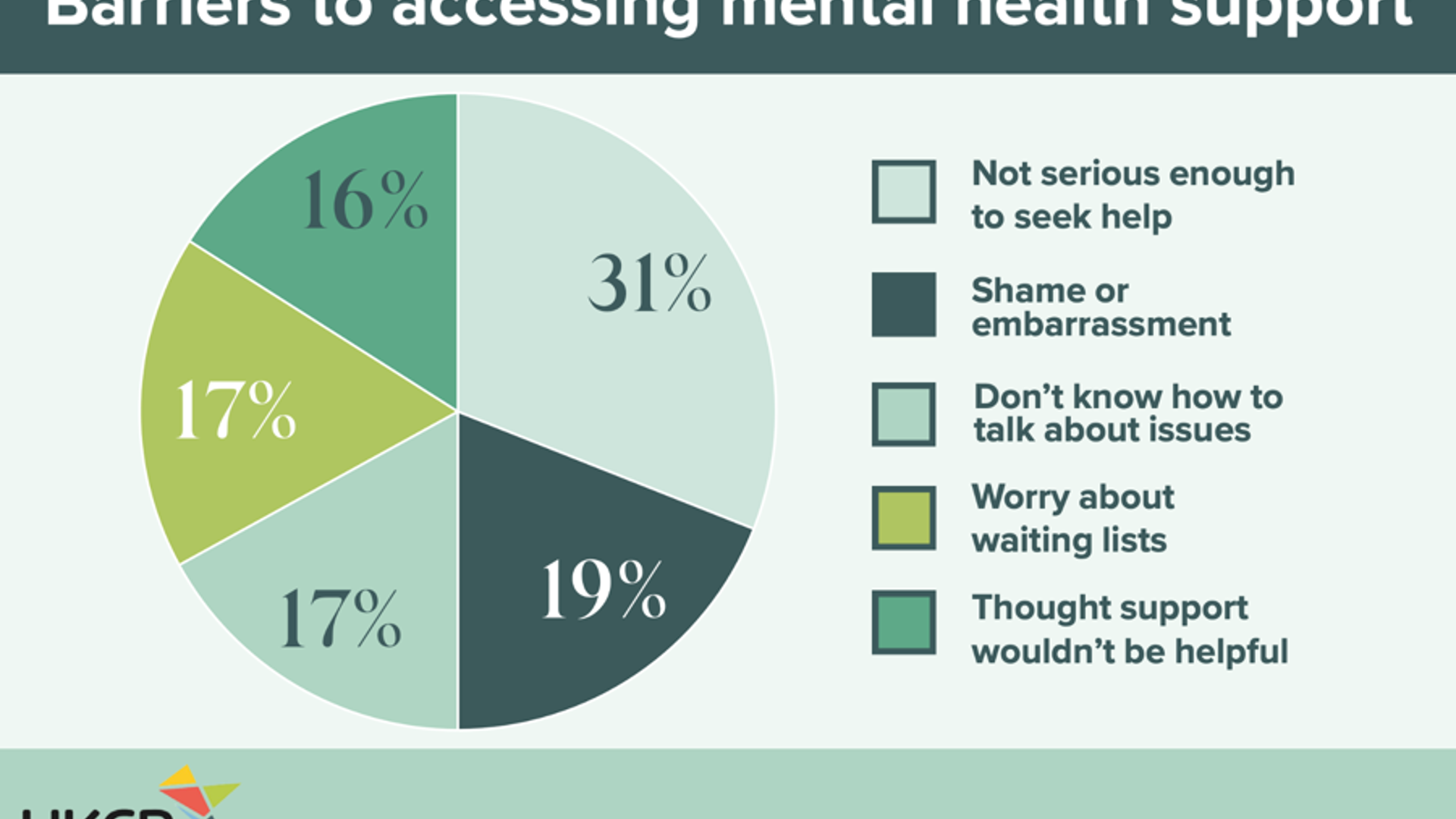
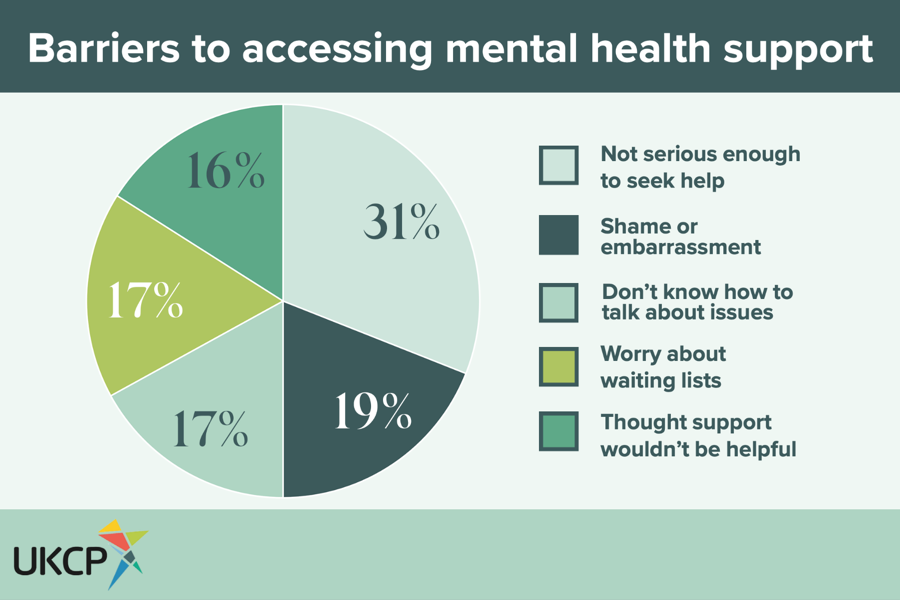
Our survey highlighted the long-lasting impact of COVID-19 on mental health. Nearly one in five respondents were concerned for their mental health following the lifting of lockdown restrictions and, of those whose mental health was impacted, more than half (57%) encountered barriers to accessing support.
One barrier frequently cited by participants was stigma, including worries that their issue was not serious enough to seek help for and feelings of embarrassment and shame. UKCP has campaigned for years for better availability of free-to-access talking therapies and on reducing barriers to access to key mental health support services, and these survey results underline how necessary this is. In addition, men were more hesitant to seek help, with significantly fewer male participants indicating that they would seek support from a GP as compared to women, highlighting the impact of gender norms on help-seeking behaviour.
For those who overcame barriers and sought support, the frontline NHS services they received often did not improve their mental health as expected. More than half of respondents found that NHS support either made no difference or worsened their mental health. The services that fell short of expectations were most frequently accessed through GPs, who act as one of the first points of access for mental health services in the UK. A lack of understanding of the prescribing options available could be a significant reason behind this trend. This highlights the importance of providing GPs with better tools to support the increasing number of their patients with mental health needs – including improving the choice of referral pathways.
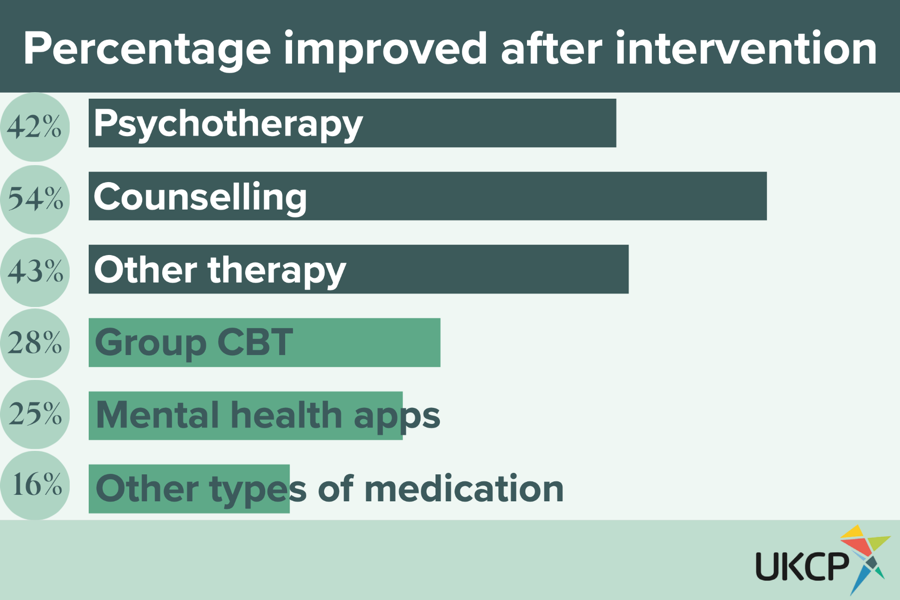
Crucially, for those who improved following mental health support, a higher percentage had received psychotherapy, counselling, and other talking therapies. In comparison, mental health smartphone apps, group cognitive behavioural therapy (CBT), and medications other than antidepressants had the lowest percentage of participants who found the support they received improved their health. Furthermore, psychotherapy and counselling were both found to be more likely to have positive outcomes than individual CBT and antidepressants, which are two of the most dominant offerings across NHS services. These figures demonstrate how vital it is to increase the range of mental health treatments available through the NHS, including significantly expanding the choice of talking therapies, to increase the possibility of positive outcomes.
These findings highlight how important it is that GPs, NHS service providers and therapists collaborate to improve awareness of the different types of mental health support available. COVID-19 and its after effects will continue to have a detrimental impact on mental health in the years to come and people must be provided with effective support to counter this. To address this urgent problem, UKCP will work with key decision makers at a national and local level, GPs, and our members to ensure a genuine choice of talking therapies available through NHS services is priority in the years to come.
Find out how this research relates to our policy goals here.

